Full article below from NACPM Board Member Farrah Ka’haleani Rivera, as posted in the NACPM April 2026 newsletter.
The word “advocacy”, while by definition encompasses an action, can mean many things to different people. I would like to speak to the intention of the why perinatal advocacy is critical to the improvement of perinatal health disparities, and highlight examples of how you can step in, too.
For many, becoming an advocate is a necessity to speak on behalf of an injustice that is witnessed and or experienced, not addressed, repeats, and is then perpetuated. In this perpetuation, generational harm can happen and possibly, in the worst case scenario, lead to the development of cultural norms — for example, ohana (family) holding the belief that the only option to birth is in a hospital setting. As a community-based midwife educator, perinatal advocate, and NACPM Board Member, I know this is to not be true. Rather, there is historical, patriarchal, and capitalistic rhetoric that lead to births being taken away from ohana and midwifery and into hospitals.
While hospital birth can be assessed as a safe option for birthing people who require higher level of care, this is not true for low-risk pregnancies who are being cared for by midwives. Instead, what can create an unsafe out-of-hospital birthing situation is the lack of access to providers who are trained and experienced to conduct adequate perinatal care (American College of Obstetricians and Gynecologists, 2023) as well as delays in treatment of emergent transfers (Team, 2025) that is largely due to the lack of integration of out-of-hospital birth, resulting in the perpetuation that midwifery is an afterthought for the care of our reproductive populations.
Access Matters
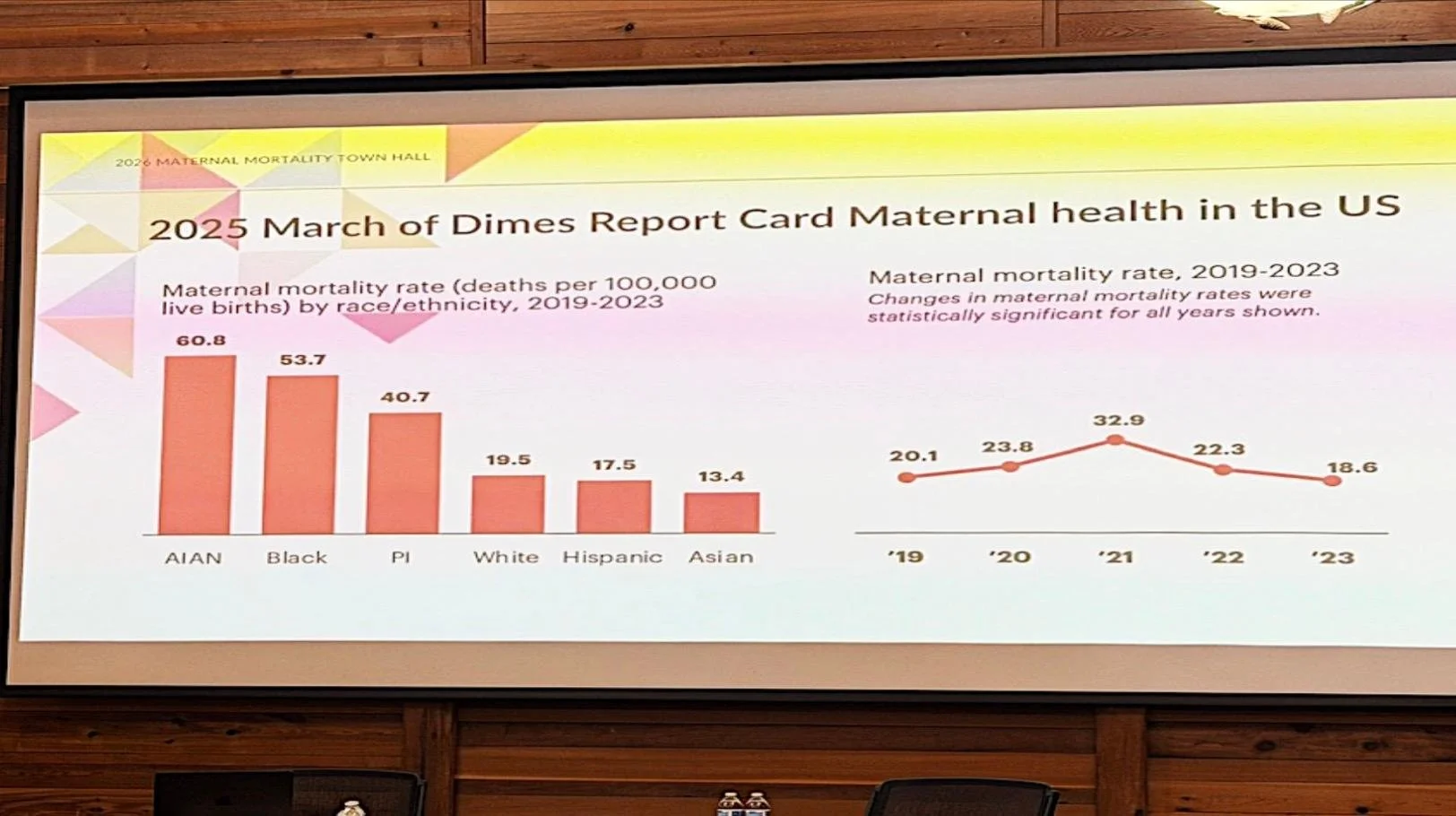
Access to providers who are trained, experienced, and culturally representative of the communities they serve ties directly into the statistics of populations who are actively experiencing higher rates of maternal death: American Indian/Alaska Native, Black, and Pacific Islander populations (March of Dimes, 2024). Research is also catching up to the community knowledge that students in midwifery education are emphasizing the need to re-envision midwifery education that includes the following (Altman et al., 2025):
Teachings of midwifery origins and history
Centering Black and Indigenous learners in midwifery education
The need for a more inclusive version of midwifery education
Increasing access to midwifery education
The diversification of midwifery workforce is not only crucial for the improvement of perinatal outcomes, but an act of reclamation for birthing communities. It also stands as a known evidence-based resolution to improve perinatal disparities (Almanza et al., 2022). However, even if we are successful in the diversification of the midwifery workforce and the increase in number of midwives, birthing people and perinatal providers are still facing the delays in treatment of emergent conditions in the perinatal period.
Delays and Lack of Integration
The full integration of midwives within maternity care systems in the United States could reduce perinatal health disparities as well as fill in the gaps where provider shortages are prominent (Niles & Zephyrin, 2023). While the demand for increasing the number midwives continues to grow, legislation, regulations that restrict autonomous practices, little-to-no federal support to fund midwifery education and training, and inequitable Medicaid reimbursement severely restrict the growth of our midwifery workforce.
As is it currently stands, hospital staff shortages and the continued closures of labor and delivery units across the nation are creating more and more maternity care deserts (Stopping the Loss of Rural Maternity Care – Saving Rural Hospitals, 2020). Centralizing hospital care access worsens delays in treatment and places intense strain on the hospital staff working in these systems (Medicus Healthcare Solutions, 2025).
We need more midwives who serve the communities they represent. We need to train and educate more midwives and create open access to this training and education. We need to do this swiftly and in ways that put midwifery care back at the forefront of being the primary providers to serve our reproductive populations. What we know is that where midwives are respected, regulated, and fully included in collaborative care, outcomes improve by reducing unnecessary interventions, enhancing psychosocial wellbeing, and supporting healthier pregnant people and their babies.
Where does your advocacy fit? Advocacy in supporting midwifery and midwifery education requires intentional actions to strengthen the profession. This can happen at any level: individually, alongside community and institutions, and on policy and legislative levels.
Supporting Midwifery Practice
Advocacy for midwifery means ensuring midwives are recognized as essential healthcare providers and fully integrated into maternity systems. This can include:
Promoting licensure and fair regulation for Certified Professional Midwives, Certified Nurse-Midwives, and Certified Midwives
Expanding Medicaid and insurance reimbursement for midwifery services
Supporting birth centers, home birth options, and collaborative hospital relationships
Educating policymakers and the public about evidence that shows midwifery improves outcomes and reduces unnecessary interventions
Addressing maternity care deserts by increasing access to midwives in rural and underserved communities
Organizations like National Association of Certified Professional Midwives (NACPM) and American College of Nurse-Midwives (ACNM) often lead this work.
Supporting Midwifery Education
Advocacy in education focuses on creating equitable pathways for future midwives. This can include:
Reducing financial barriers through scholarships, grants, and loan support
Expanding apprenticeships, distance learning, and multiple educational pathways
Recruiting and retaining diverse students and faculty
Protecting accreditation standards while keeping programs accessible
Integrating anti-racism, cultural humility, reproductive justice, and community-based care into curricula
Supporting preceptors and clinical placement opportunities
What advocacy ultimately looks like is building a future where every family can access qualified midwifery care, and every aspiring midwife has a fair chance to become one.
References
Almanza, J. I., Karbeah, J. ’Mag, Tessier, K. M., Neerland, C., Stoll, K., Hardeman, R. R., & Vedam, S. (2022). The Impact of Culturally-Centered Care on Peripartum Experiences of Autonomy and Respect in Community Birth Centers: A Comparative Study. Maternal and Child Health Journal, 26(4), 895–904. https://doi.org/10.1007/s10995-021-03245-w
Altman, M. R., Washington, T., Uthmaan, S., Akoma, M., Niang, B., Gilmore, C., Monk, L. S., Kennedy, L., & Fletcher, V. (2025). Understanding Perspectives of Midwifery Education from Black and Indigenous Community Stakeholders: “We’re Working in a System That Was Not Intended for Us.” Journal of Midwifery & Women’s Health, 70(6), 889–896. https://doi.org/10.1111/jmwh.70057
American College of Obstetricians and Gynecologists. (2023). Planned Home Birth. Acog.org. https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2017/04/planned-home-birth
March of Dimes. (2024). 2024 March Of Dimes Report Card For United States. March of Dimes | PeriStats. https://www.marchofdimes.org/peristats/reports/united-states/report-card
Medicus Healthcare Solutions. (2025, August 21). Insights Into the OB/GYN Shortage: Understanding the Supply and Demand Gap. Medicushcs.com; Medicus Healthcare Solutions. https://medicushcs.com/locum-tenens-agency/resources/insights-into-the-ob/gyn-shortage-understanding-the-supply-and-demand-gap
Niles, M., & Zephyrin, L. (2023, May 5). How Expanding the Role of Midwives in U.S. Health Care Could Help Address the Maternal Health Crisis. Www.commonwealthfund.org. https://www.commonwealthfund.org/publications/issue-briefs/2023/may/expanding-role-midwives-address-maternal-health-crisis
Stopping the Loss of Rural Maternity Care – Saving Rural Hospitals. (2020). Chqpr.org. https://ruralhospitals.chqpr.org/Maternity_Care.html
Team, B. L. (2025, October 20). Birth Risks At-Home vs a Hospital | Chicago Birth Injury Law. Beam Legal Team. https://www.beamlegalteam.com/blog/what-are-the-risks-of-at-home-births-compared-to-hospital-births/